Eczema
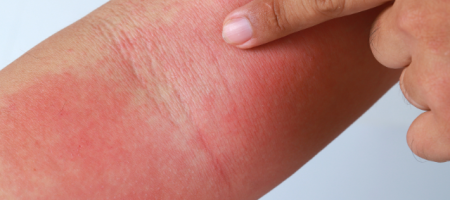
Atopic eczema, also known as atopic dermatitis, is a chronic (long-term) skin condition that causes itchy and inflamed skin. It most commonly begins early in life affecting infants and young children but may occasionally begin in adulthood.
Symptoms
Atopic eczema presents as generalised skin itching and rash. Early on the skin may become red, swell, bubble up and weep. Longer term the skin may become dry and thickened.
The rash will typically appear in babies on the face. In toddlers and older children they tend to affect skin creases such as the inside of the elbows and behind the knees. It may also appear elsewhere on the skin.
Causes
Atopic eczema is due to a combination of your genes and immune system interacting with your environment. In atopic eczema, the skin cannot act well as a barrier to keep moisture in and germs and substances from the outside world out.
Because of this, water/moisture leaves the skin, causing it to dry very easily leading to cracking and itching. Scratching then further breaks down the barrier in a vicious cycle.
Treatments
The first step in treating atopic eczema is avoiding these aggravating factors:
- Rubbing and scratching
- Skin irritants such as sweat, soaps, detergents, and prickly clothes.
- Long hot showers that can remove the natural oils from the skin and cause moisture loss. It is better to have short, lukewarm (around 32°C) showers.
- Indoor heating dries the skin in winter, and coarse and rough clothing can irritate the skin.
- If there are known allergies, avoid or minimise exposure as much as possible.
Following that, topical treatments are the mainstay of managing atopic eczema. Topical treatments include prescribed medicated gels, creams or ointment and moisturisers in the form of lotions, creams and ointments applied directly to the skin. Wet wraps may be added. Most people respond very well to topical treatments and often do not need any other types of treatment.
Secondary infections from bacteria and viruses are treated with antibiotics and antivirals.
Other treatments given to patients that aren’t responding to topical treatments only include:
- Light treatment (phototherapy)
- Oral medications:
- Injectable medications (biologics).
Resources
For further information, you can visit the following resources:

