Psoriasis
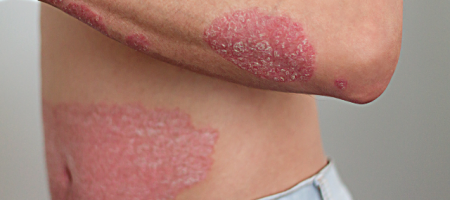
Psoriasis is a lifelong skin condition characterised by the development of red, scaly, thickened areas of skin. About 50% of people affected with psoriasis have changes to their nails and about 25% of people have pain, swelling and tenderness of their joints.
There are several different types of psoriasis. Chronic plaque psoriasis (psoriasis vulgaris)
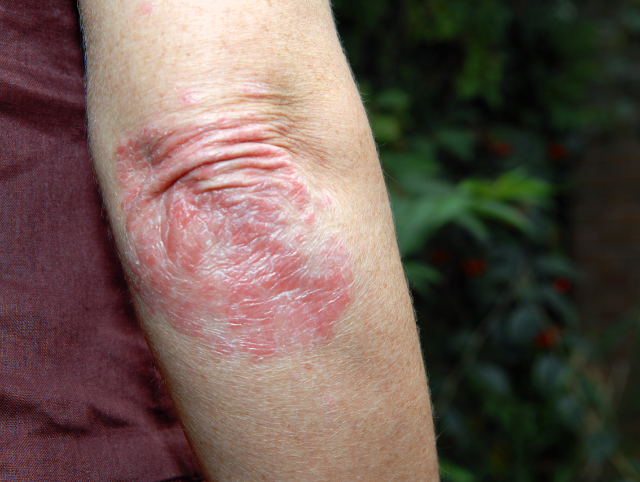
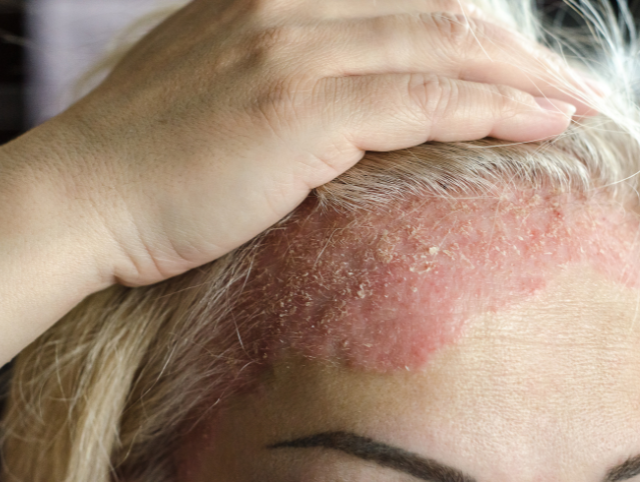
Chronic plaque psoriasis occurs in 90% of people affected by psoriasis. It has characteristic thick, sharply edged (marginated) red scaly lesions. It may be seen on any area of the skin, but the elbows, knees, lower back and scalp are most commonly affected by the condition. The affected areas may be itchy or mildly uncomfortable.
Less common forms of psoriasis include:
- Inverse (flexural) psoriasis occurs in the armpits, groin, between the buttocks, in the belly button (umbilicus), the ears and other areas where skin rubs against skin. It has characteristic sharp-edged patches with little or no scale.
- Palmoplantar psoriasis occurs on the palms of the hands or soles of the feet. It has characteristic scaling, redness or pustules (small blister or pimple on the skin containing pus).
- Guttate psoriasis is most commonly seen in young adults 2 to 3 weeks after they have had tonsillitis or a viral infection. It develops rapidly and has characteristic widespread, small, thin, teardrop lesions. It usually improves over a period of 2 to 3 months.
- Pustular psoriasis is a very rare form of psoriasis which appears suddenly and presents as small pustules developing in inflamed skin and spreading rapidly. The person is sick, and hospitalisation and oral medications are necessary.
- Erythrodermic psoriasis is a rare, severe form involving almost the entire skin surface. This is considered a medical emergency and requires prompt treatment, sometimes in hospital.
- Nail psoriasis can affect the nails in several ways, including with pitting or grooves in the nails, thickening, yellow discolouration, detachment of the nail plate off the nail bed (onycholysis), or discoloured spots in the nail bed. It may affect just one or a few nails or all fingernails and toenails.
Causes
The exact cause of psoriasis is unknown. It is thought that psoriasis develops in people who have an inherited tendency for the immune system in their skin to react abnormally to certain environmental conditions.
Psoriasis is more common in people who have relatives with psoriasis. The condition affects all racial groups and affects about 2% of people worldwide.
Psoriasis may be triggered for the first time by infections such as streptococcal tonsillitis, HIV and other viral infections as well as by severe emotional stress. Psoriasis is not contagious.
Smoking and excessive alcohol intake may worsen the condition.
Some medications may trigger psoriasis or cause psoriasis to become more severe. These medications include lithium, beta-blockers, anti-malarial medication, and rapid withdrawal of systemic corticosteroids.
Treatments
General measures:
- Daily application of moisturiser to all of the skin is essential to maintain skin hydration and barrier function.
- Improve lifestyle factors: stop smoking, avoid excessive alcohol intake and excess weight gain.
- It is important not to withdraw from social contact and activities because of the psoriasis.
- Join a psoriasis support group and share concerns with family members and other people affected by psoriasis.
- Discuss any anxietyor depression with a
Specific treatments:
- Topical treatments
- Corticosteroids
- Vitamin D preparations (calcipotriol or calcipotriol combined with a topical corticosteroid)
- Tazarotene
- Coal tar
- Dithranol
- Ultraviolet (UV) phototherapy and photochemotherapy
- Narrowband UVB
- PUVA
- Systemic treatments
- Methotrexate
- Cyclosporin
- Retinoids
- Biologic agents
Resources
For further information, you can visit the following resources:

